The discovery of antibiotics – notably by Alexander Fleming in 1928 – was a major milestone in medicine. Antibiotics save countless lives. For years, they have been used to fight bacterial infections, including streptococcal infections in cases of tonsillitis or E. coli infections in cases of cystitis.
But they are also used preventively, for instance in the context of surgical interventions or chemotherapy, because in these situations the risk of bacterial infection is higher, which can lead to complications. Antibiotics are also used in veterinary medicine.
However, over the past 30 years, an increasing number of bacteria have become resistant to certain antibiotics. This means those antibiotics are no longer effective against them. Some bacteria are resistant to nearly all antibiotics, which is why they are known as ‘super bugs’.
In other words, some bacterial infections can no longer be treated as effectively, or can no longer be treated at all.
In 2019, around 1.3 million people worldwide died from infections caused by bacteria that were resistant to antibiotics, twice as many as died of malaria or HIV.
A recent study predicts this number could rise to 1.9 million per year by 2050.
Some forecasts are even more dire.
The WHO lists antibiotic resistance as one of the top 10 threats to global health and the EU also ranks it among its three most critical challenges.
But why does resistance develop in the first place? What is the situation in Luxembourg? And what progress is being made in developing new treatments?
For this video, we gathered advice from experts including Jacques Zimmer, researcher at the Luxembourg Institute of Health, and from members of the 'Monitoring' working group of the Health Directorate’s National Antibiotics Plan.
Bacteria are tiny microbes that help us with many things, for example, digesting our food. But some can also make us sick, similar to how viruses do. However, and this is key: bacteria are not viruses. That is why antibiotics are not effective against viral infections, which is what most colds are, for example.
Just like viruses, however, bacteria continue to evolve through genetic mutations to survive. Sometimes, these mutations enable them to withstand antibiotics. As a result, new resistant strains of bacteria emerge and gradually spread. This is a natural process that we can't prevent: evolution.
As already mentioned, antibiotics save many lives, but unfortunately, they're sometimes prescribed unnecessarily.
For example, when they are prescribed for the flu or colds that are caused by viruses.
Another example is the use of antibiotics in livestock for economic reasons, for example, to allow animals to be kept in smaller spaces to keep meat prices low.
The good news is that antibiotic use in Luxembourg has decreased over the last ten years: the entire health sector now uses about 25% less.
We are now roughly in line with the EU average.
In livestock farming, antibiotic use has almost halved compared to ten years ago.
In this respect, Luxembourg is now among the EU countries with the lowest antibiotic use – nearly three times less than Germany or Belgium.
And what about resistance to antibiotics?
In terms of resistance, early indicators suggest that the situation has somewhat stabilised in Luxembourg. However, data on this remains limited, so no general conclusions can yet be drawn.
In the healthcare sector, resistance was observed, for example, in ten bacteria-antibiotic pairs between 2018 and 2022, based on samples from hospitals where patients had bloodstream infections or infections of the central nervous system.
For most of the ten bacteria-antibiotic pairs analysed, the proportion of resistant bacteria has remained stable or has slightly decreased in recent years, with a few exceptions. There are also cases where it is increasing. And it should be emphasised that in some cases, the proportion of antibiotic-resistant bacteria – even if it is decreasing – remains high. For example, 50% of E. coli strains are resistant to the common antibiotic aminopenicillin. Resistance thus makes it harder to treat common infections.
The evolution of resistance is also monitored in veterinary medicine. In this area, the proportion of resistant bacteria remains high in many cases analysed, but it has remained stable in recent years.
In Luxembourg, the trend is going in the right direction, but the proportion of resistant bacteria remains very high in many cases.
The development of resistance to antibiotics is, of course, a global phenomenon and there are major differences between countries in terms of antibiotic consumption and resistance development.
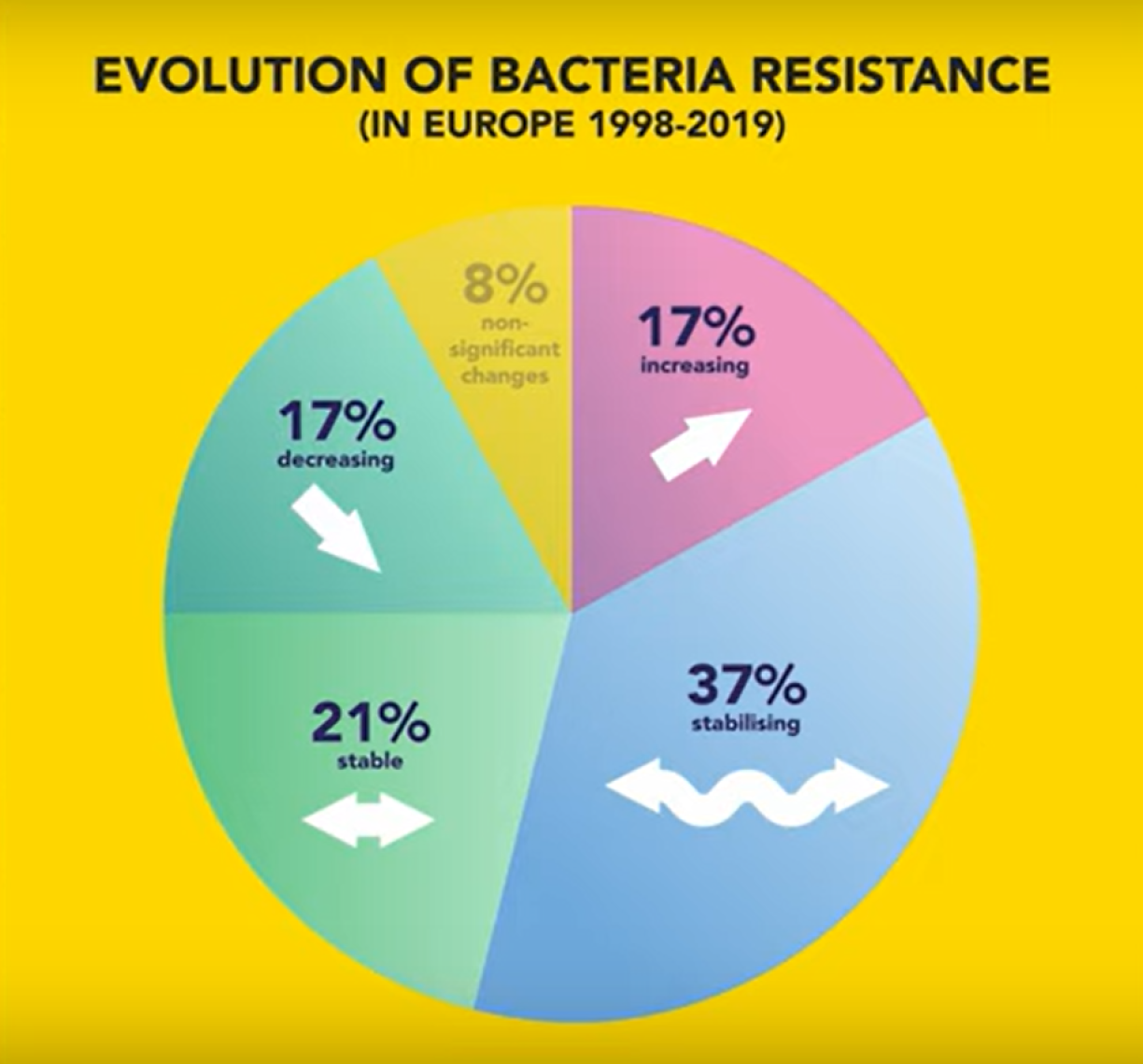
Europe also appears to be moving in the right direction. In 50% of the analysed bacteria-antibiotic pairs, the proportion of resistant bacteria has more or less stabilised over the past 20 years.For 17% the proportion continues to rise and for 17% it is decreasing.
This was discovered by researchers in an overview study, which, however, has not yet been peer-reviewed.
Still, the WHO warns of “alarming” levels of resistance worldwide.
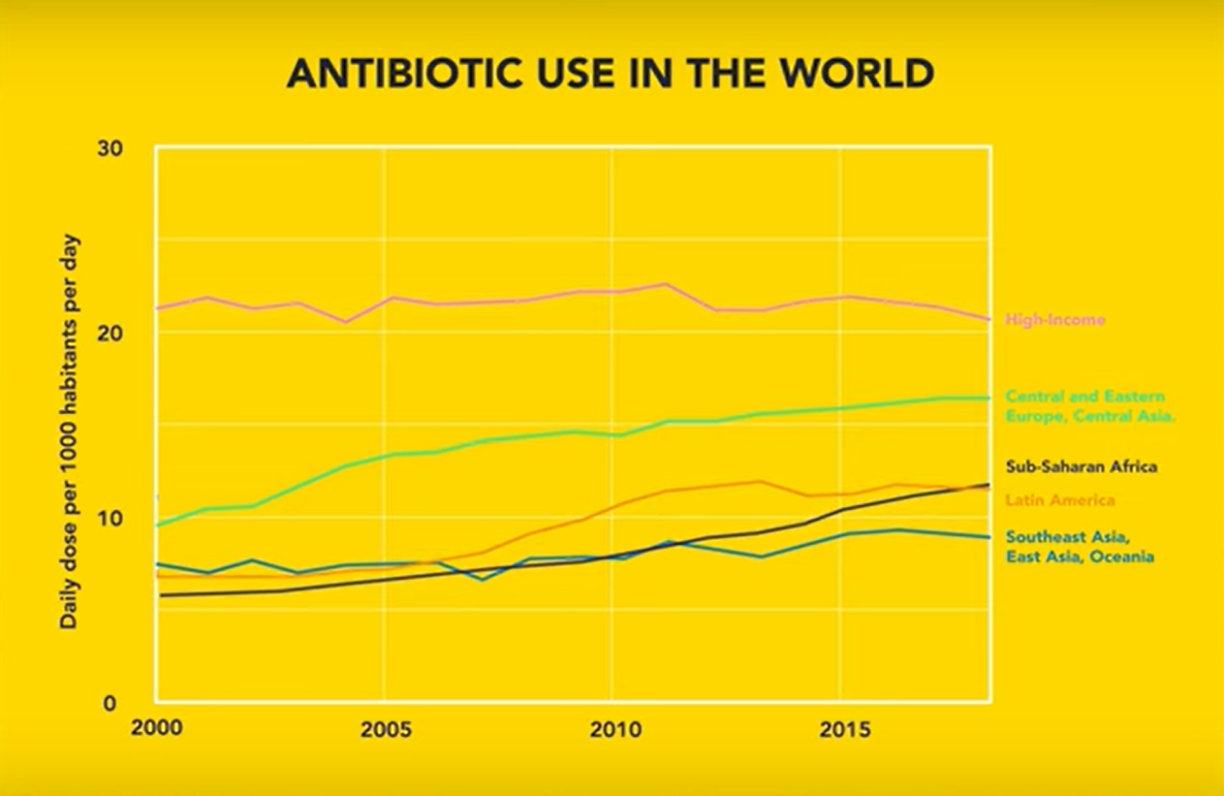
In North Africa, the Middle East and South Asia, antibiotic consumption has nearly doubled over the past 20 years. On the one hand, this is of course positive for the health of local populations, but it also leads to the development of new forms of resistance that can spread everywhere in our globalised world.
From a global perspective, however, the situation is still far from being under control.
Despite great efforts to reduce antibiotic consumption, the truth is that resistant bacteria will never just disappear by themselves. And that brings us to another critical point: We urgently need new antibiotics and/or alternatives.
Only a few new antibiotics have come onto the market in the past 50 years. On the one hand, because it is difficult to find new ones, but also because it is not a lucrative business.
The development of an antibiotic takes on average 12 years and costs 1.5 billion dollars.
A patient typically uses antibiotics for just a week, a short time from a commercial perspective. Additionally, every new antibiotic is initially placed on a backup list and prescribed only when no other option is effective. This means sales are minimal.
Adding to the challenge, resistance to new antibiotics can develop quickly, sometimes even before the drug reaches the market.
Nevertheless, the search for new antibiotics or alternative treatments must go on.
In Luxembourg too, researchers like Jacques Zimmer are exploring alternatives to antibiotics, such as immunotherapies, where our own immune cells are stimulated to target and kill bacteria directly.

While we aren't on the brink of a global catastrophe due to ‘super bugs’, the situation is still serious.
We cannot stop bacteria from developing resistance, but we can slow the process. This means using antibiotics only when absolutely necessary.
We can all contribute to that.
And if research into new antibiotics and alternatives continues, we can hopefully stay ahead in the fight against bacteria.
Ziel mir keng! is broadcast on Sunday evenings after the programme Wëssensmagazin Pisa on RTL Tëlee and is a collaboration between RTL and the Luxembourg National Research Fund. You can also watch the episodes on RTL Play.
Author: Michèle Weber (FNR)
Editing: Lucie Zeches (FNR)
Advice: Jacques Zimmer (LIH), National Antibiotics Plan (PNA) (Health Directorate)
Background research and infographics: Daniel Saraga (saraga communications)
Video and design of the infographics: SKIN
Translation: Nadia Taouil (www.t9n.lu)